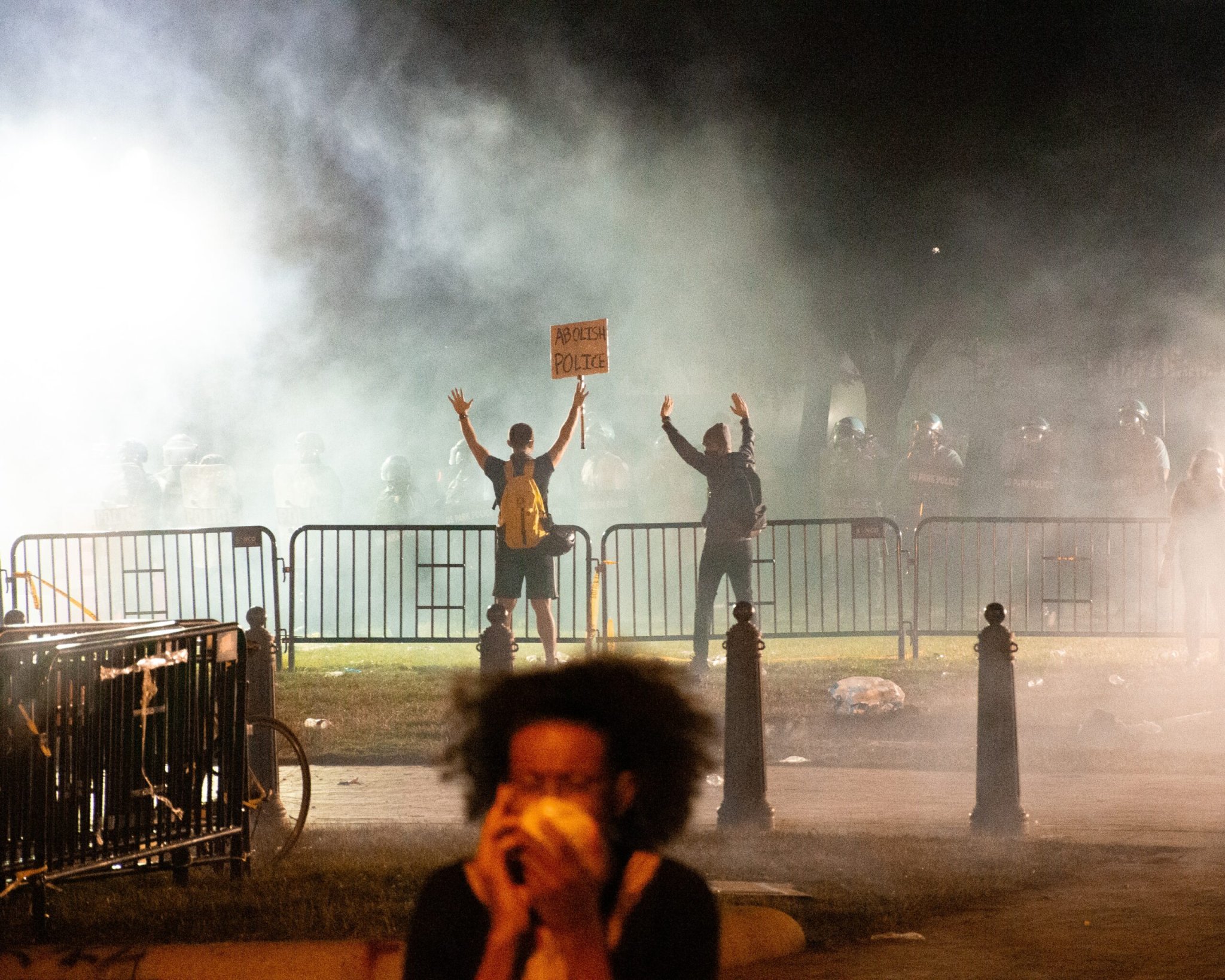
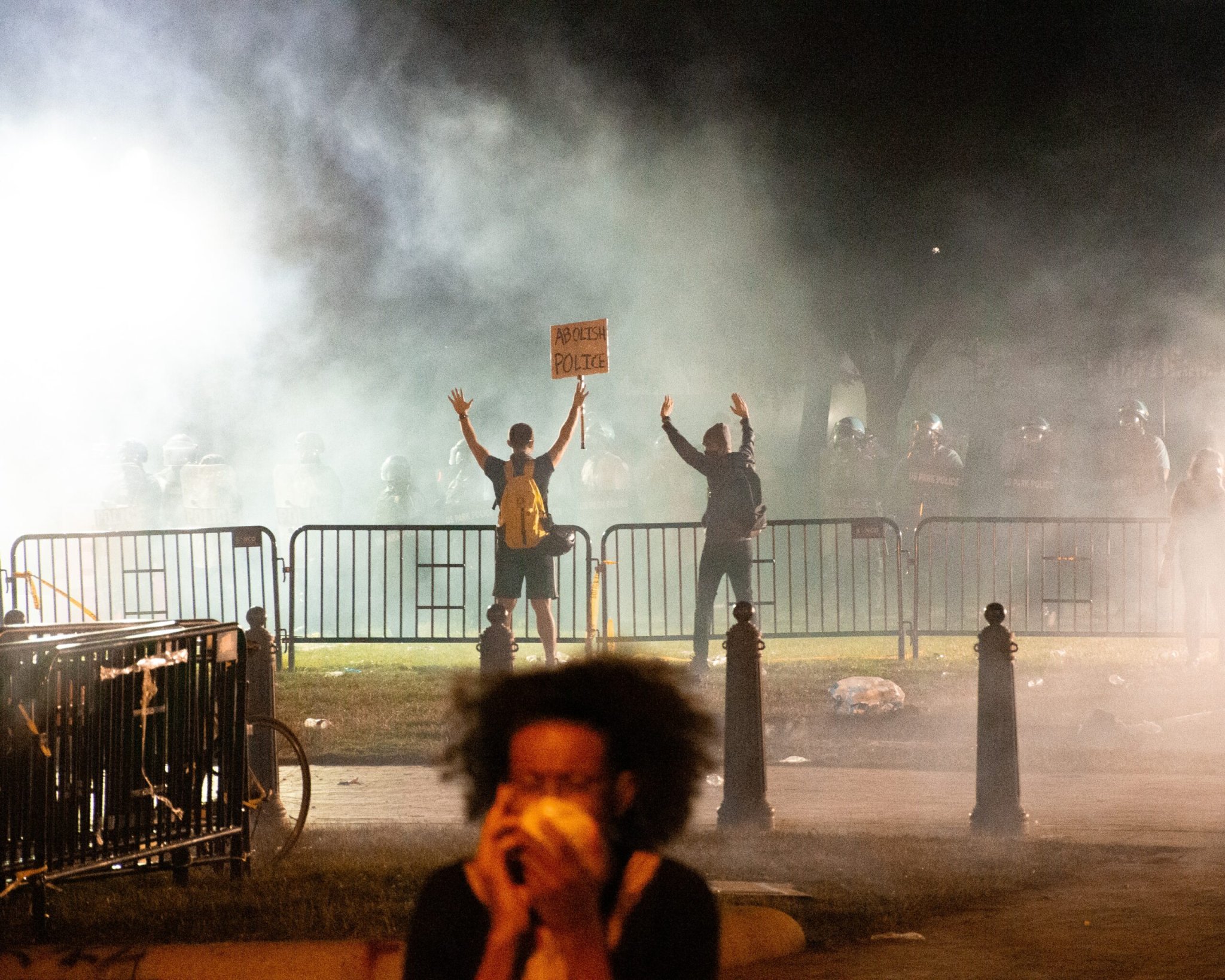
Grey clouds waft over scattering crowds in the footage from Seattle this past Sunday. The yells and screams of police and protesters alike are punctuated by shots of flare guns. Eventually, the street empties out, but the haze of tear gas continues to swirl under the lights.
As more and more dissidents take to the streets in solidarity with Black Lives Matter, US police have unleashed some dangerous crowd-control tools, possibly exacerbating the continued health risks of COVID-19. Cities like Seattle are still seeing hundreds of new cases each week—and doctors worry that dispersing mass amounts of tear gas could needlessly damage people’s lungs and cause greater risk of virus exposure.
“The coronavirus is still quite active … and we will likely see a rise in cases,” says Anna Nolan, a pulmonologist at New York University School of Medicine who’s been treating COVID-19 patients. “It’s unfortunate, but true.”
Whether a person is exposed to tear gas and then SARS-Cov-2, or they’re recovering from the virus and subsequently get gassed, Nolan says the two make a terrible combination, given the damage they inflict on internal organs. Research on tear gas, which is often made of a powdered irritant, links it to a slew of respiratory conditions, including choking, blistering, bronchitis, pneumonia, chest pain, and long-lasting lung damage. In fact, the Chemical Weapons Convention deemed tear gas so harmful that they banned it from international war in 1993.
“If exposure to tear gas is prolonged, it can result in pretty severe respiratory impacts,” says Howard Hu, an epidemiologist at the University of Washington who’s studied global tear gas use and its effects. He says there are many well-documented cases of people developing asthma after living alongside it for days, and adds that it can worsen deadly pre-existing conditions like emphysema, hypertension, and coronary artery diseases.
In 2013, 37 detainees in Egypt died from asphyxiation from tear gas. And just today, the city of Columbus, Ohio, launched an investigation of the death of a 22-year-old protester who was hospitalized after being tear gassed.
Considering that COVID-19 causes respiratory distress and failure in many patients, Nolan says that people being pushed into crowds and small spaces while being exposed to a breathing-impairment tool is “really problematic.” But as far as the compounded effects of tear gas and coronavirus, that’s still an open question.
“If you irritate the airways further [with tear gas], will you get predisposed to COVID-19? That’s a thought,” Nolan says. “Nobody’s really looked at that combination yet, but I’m sure we will know more about that over the coming weeks if this type of activity continues.” For now, Nolan and other doctors are warning protestors with underlying lung conditions to stay vigilant: If they do contract the virus, they may experience severer symptoms.
Assessing long-term risk is complicated, though, because the lasting effects of tear gas haven’t been adequately documented. “There really is no decent research that’s been conducted on communities exposed to gas,” Hu says. “When this was first developed by the US Army, all the research was conducted on healthy men—they weren’t exposed to really high concentrations, nor were they followed for months or years.” But for a lot of the communities that are currently marching and protesting, there may be a days-long period of exposure. “We’re in uncharted territory,” Hu adds.
As protesters and police funnel into residential neighborhoods, clouds of tear gas are also entering people’s homes—a hazard for anyone staying indoors to avoid the virus. The chemical can stick to clothing and skin for up to 72 hours, and has deadlier consequences when it builds up in enclosed areas.
“There are case reports that in neighborhoods where tear gas was used, the people inside were really stuck,” says Rohini Haar, an emergency physician and health and human rights researcher at UC Berkeley. “The best way to get rid of it is to open your windows and let in fresh air. But if that makes more tear gas come in, then there’s really no safe air to breathe.”
“It’s supposed to be a weapon of last resort,” Haar goes on to explain. Originally, it was intended for dispersal at the periphery of crowds, but the police have been going beyond that by “firing too many canisters, targeting the canisters to hit people directly in the middle of the crowd, or using it in enclosed spaces.” “For them to continue to use excessive amounts of tear gas when people have to wear masks is very irresponsible,” Haar adds. Videos circulating on Twitter show protesters removing their masks after being gassed to get a few breaths of air; others reveal officers pulling down protestors’ masks to pepper spray them directly in the face. At least 1,300 health professionals recently signed an open letter opposing the “systemic injustice occurring during the COVID-19 pandemic,” urging police departments to halt the use of tear gas.
In the chaos of a protest, with crowds running and regrouping, it becomes nearly impossible to maintain COVID-19 safety measures. Nolan worries about the health of both protestors and coronavirus patients down the line: “As a pulmonologist, knowing what I know … it’s so clear that not using those inhalation irritants on people who are peacefully protesting would limit risk.”
“The science is not moving the policy the way it should,“ Haar says, alluding to the fact that the dangerous side effects of tear gas have long been known. “Both police violence and health services are due for a reckoning around race and disparities as much as every other system in the US. Being in the era of coronavirus makes that an even more urgent need.”
