We may earn revenue from the products available on this page and participate in affiliate programs. Learn more ›
What if you could walk into a grocery store, scan the barcode on a Rice Krispie treat, and find out how it would affect your blood sugar before buying it? That’s the promise of January, a virtual continuous glucose monitor (CGM) system that the company describes as a “24/7 AI health coach to change the way you live.”
As a middle-aged woman with a family history of diabetes and a pizza weakness, I’ve wanted to try a CGM. After more than a week of testing the January AI system, I found it to be an effective tool that gave me more insight into my metabolic health and actually helped me lose a few pounds. It’s a sizeable investment but can return equally valuable insights if you sign up for a subscription and keep a few things in mind.
January
See ItPros
- Provides feedback in real-time on how various foods will affect your glucose levels
- Includes a comprehensive database of foods. You can also enter using a QR code on-site in a store
- Fun to use
- Recommends activity to counteract high glucose levels
- Provides meal plans and activity recommendations based on your nutritional needs and preferences
Cons
- Somewhat expensive
- Might not be good for someone with a history of disordered eating around calorie restriction
- Sensor came out somewhat easily
Overview
- After filling out your health history in an online telehealth session, if you’re approved, January will send you a CGM
- Once you attach the CGM to your arm, you log the food you’ve eaten, scan the sensor with your phone, and the January app shows your glucose levels in real-time
- You must also sync with an Apple Watch or an Oura Ring to record your activity levels
- After five days, January will provide detailed recommendations for foods to eat and activities, taking your preferences into account
- A one-month subscription costs $288,and an annual subscription is $380
Verdict: If you’re concerned about your risk of diabetes because of family history, physical health, or age, or you just want personalized recommendations on how to live healthier, the January AI system is a useful and fun tool.
What is a continuous glucose monitor (CGM)?
Continuous glucose monitors were originally developed in the 1980s to help diabetics keep tabs on their blood glucose, or blood sugar, levels. People with diabetes have trouble making insulin, a hormone secreted by the pancreas that allows glucose to be used by cells for energy. Glucose then remains in the bloodstream, keeping blood sugar levels high over time. Chronic high blood sugar can also damage the kidneys, heart, and nervous system.
While CGMs used to require users to prick their fingers to test their blood sugar, newer CGMs include a small sensor that goes under the skin. The sensor will then transmit readings of your glucose levels to a device that will analyze them. Pioneering CGM makers include Dexcom, which made the first CGM that didn’t require a finger pricking and got FDA approval for diabetics in 2016.
Increasingly, people who aren’t diabetic, including elite athletes, are using CGMs to get a more granular sense of their metabolic health. Other popular CGMs that keep popping up in my Instagram feed include Nutrisense and Levels. Tech sites have speculated for years about Apple’s possible plan to build a CGM into the Apple Watch. However, CGMs still require a medical prescription, and their use by people who haven’t been diagnosed with diabetes has generated debate in the medical community. One perspective published in the journal JAMA described CGMs for non-diabetics as a “waste of time and money.”
Other doctors point to the more than 120 million Americans who either already have diabetes or are prediabetic. Peter Attia, M.D., who co-authored the bestselling book, Outlive: The Science and Art of Longevity, makes the case that the typical blood sugar tests that patients get annually don’t reveal daily spikes that can signal a brewing problem.
“In the vast majority of cases, today’s normal individual is tomorrow’s diabetic patient if something isn’t done to detect and prevent this slide,” Attia writes. Fluctuating glucose levels have also been associated with an increased risk of heart disease, cancer, and Alzheimer’s disease, he notes.
While I’m generally healthy, I was interested in learning more about my blood sugar levels and how they might affect my life. My parents had been diagnosed with Type II diabetes in their 40s, so I checked the family history box. After losing weight early in the pandemic, I put on some pounds last year. And despite training for my first marathon, I found that all the exercise wasn’t helping get me into better shape as easily as running did when I was younger.
True, the lab results from the last time I was tested after a visit to my primary care doctor in September 2022 passed muster. My glucose level of 87 milligrams per deciliter (mg/dL) was in the middle of the normal range, but my hemoglobin A1C—the standard test that measures the average of blood glucose over 90 days—was 5.5%, on the high side of normal.
According to the CDC, a reading of 99 mg/dL or lower is normal for fasting blood sugar, while 100 to 125 mg/dL signals that you’re prediabetic, and 126 mg/dL or higher indicates you have diabetes. Would seeing those spikes on my phone just after eating help me make better decisions?
The background
Monitoring daily fluctuations in blood sugar can provide a much better window into your metabolic health, says Noosheen Hashemi, January’s co-founder and CEO. She became passionate about a more holistic approach to health care after learning the truth about her parents’ medical conditions. Doctors failed to diagnose her father with prostate cancer while he was being treated for another cancer. And her mother’s heart failure was misdiagnosed as asthma.
“Once you fall into that sick journey, all sorts of things can happen to you,” Hashemi says. “So I became obsessed with: ‘How can we know sooner, what can we know, and why do we know so little?’”
She teamed up with Michael Snyder, Ph.D., chair of Genetics and Director of Genomics and Personalized Medicine at Stanford School of Medicine. Snyder was conducting research that revealed a population of people who looked to have healthy blood sugar levels actually frequently had spikes in which their glucose reached diabetic levels.
“He believed this was a ticking time bomb and that we should look into it,” Hashemi says. “That’s how we got started.”
That was more than five years ago. They’ve since used machine learning to develop a library of foods complete with nutritional information and incorporated data from their clinical studies and thousands of users to develop and refine models for predicting glucose spikes.
They also realized that most of the their users were not diabetics, but instead what Hashemi describes as “optimizers and discoverers”: fit people looking to optimize their health or people who had potential risk factors, such as a family history, like me. Hashemi is optimistic that the FDA will approve CGMs for non-diabetics next year.

The setup
People interested in using January have to complete a telehealth evaluation online. The process involves filling out an online form, not a virtual interaction with a live healthcare professional.
For $288 ($260 for the gear and $28 for the membership), you get a Freestyle Libre CGM, access to January AI’s glycemic food database and recommendations through its app, and $40 off an Oura Ring (Gen 2 or Gen 3) to track your activity. (You can also use an Apple Watch, which I did.) If you’re approved, the Freestyle Libre will arrive in the mail shortly.
Easy-to-follow videos on the Freestyle LibreLink app showed me how to apply the CGM sensor. I felt a slight pin prick and mild soreness when I installed the sensor on my left upper arm. The app is connected to a medical practice based in California. After agreeing to use of my health data, I was up and running.
Then using the January app, I was instructed how to scan the sensor with my phone and sync my Apple Watch. Once the sensor is active, it’s ready to deliver real-time glucose readings after each scan. Over the next five days, January’s AI would analyze my glucose levels, activity, and what I was eating and compare it to its thousands of users to predict my body’s response to various foods and exercise. “It takes inputs from your heart rate monitor and your food log and your CGM to build a digital twin for you,” Hashemi says.

The performance
I began using January at the end of June, logging my meals and scanning the CGM. I found the food database reasonably comprehensive, although sometimes it took some scrolling down to find the exact food.
I was warned that the initial glucose levels could be either high or very low within the first 24 to 48 hours as the CGM calibrated to my system. My first blood sugar reading was very low—58 mg/dL—which got me googling hypoglycemia.
Then I ate a small bowl of vegetable ramen leftover from a night out at a restaurant the night before. I scanned the CGM with my phone about 5 minutes after eating and found my glucose was in the normal range: 90 mg/dL.
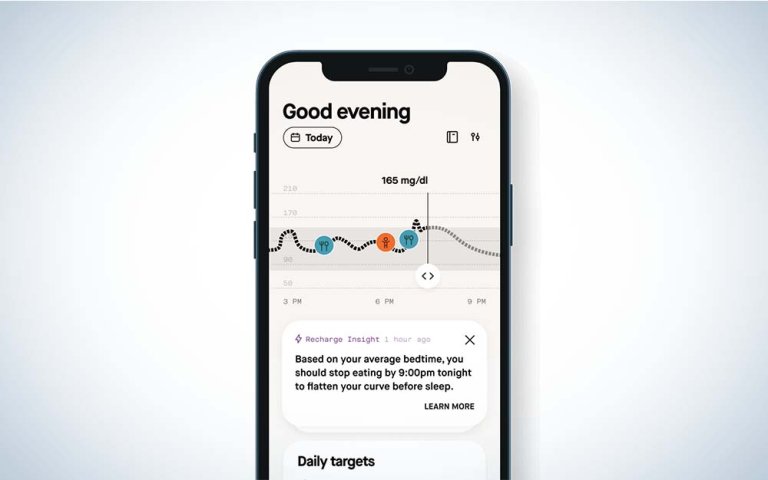
The January app provides reports on the previous day in three categories: Nourish (calories, fiber intake, and macros); Move (post-meal activity, time exercised, and calories burned); and Recharge (fasting period, last-meal sleep gap, and sleep duration). After the five initial days of analysis, January’s AI notified me that it had created my digital twin and began making recommendations for food choices and activity.
I’ve never stuck with food logs in the past, but the ability to quickly see how specific items affected my blood sugar became something I looked forward to testing. I also discovered that requirement to log what I was eating provided additional incentive to eat better. I had been prioritizing protein over refined carbs over the past few months and was glad to see that eating Greek yogurt, flax seeds, and blueberries for breakfast got me a shoutout for protein and fiber goals. I also dialed back on the snacking that’s too easy to do when working from home about six feet from the fridge.
I felt compelled in the name of science to see how a slice of pesto pizza and a Rice Krispie treat would affect my readings. As expected, these foods spiked my blood sugar more than my virtuous breakfast. When I had a high reading, the app recommended a walk after the meal. The January app also provided alternatives based on your preferences (although I was wasn’t excited to replace chia seeds with dried spirulina).
You can also reach out through the app to a virtual health coach named Jan, who provides chatbot answers on everything from what you should eat for lunch to creating a new exercise plan. The company is also in the process of adding more FAQs, such as what is a normal glucose level. Hashemi is quick to point out, however, that January is not a healthcare provider, but it does provide lifestyle recommendations based on their (and your) data.

In fact, January has explicit behaviors that it’s leading users toward, including adopting intermittent fasting, increasing fiber consumption, aligning calorie intake with activity level, getting post-meal movement, and reducing glucose-spiking foods.
I was doing reasonably well with all of these, but unfortunately, after eight days of testing, I accidentally dislodged my sensor while getting dressed. But January’s AI still provided plenty of valuable insights during the time I used it. My blood sugar was mostly low to normal, but I did see a few spikes that took me out of my normal range. And I did lose a few pounds and came to appreciate the importance of better discipline and regular meals. I did wish there was more information for people with readings on the low side.
But while the nudge toward intermittent fasting might be helpful for many (myself included), I saw how it could also cause problems for people with a propensity for disordered eating around calorie restriction. It concerned me that after I stopped logging meals, the app indicated on days when I didn’t enter food that the number of calories I consumed was “excellent.”
So, who should buy the January system?
Yes, $288 for a month’s subscription sounds expensive. But if you generally eat the same things, 30 days will give you plenty of time to analyze your health data and see how different foods affect you. I’m hopeful that glucose level monitoring will become more accessible and affordable, bearing in mind the estimated 96 million Americans over age 18 characterized as prediabetic.
Technological advances have made it possible for us to see our heart rate with a quick glance at our wrist, a luxury many of our parents didn’t have. Now, the ability to test our blood sugar is now almost as frictionless as posting on Instagram. If you’re concerned about your glucose levels due to family history or just want to fine-tune your health, January’s AI can help with daily insights and personalized recommendations. Just remember that it’s a tool and doesn’t replace regular visits to your healthcare provider.