
Science does not yet really understand the underlying causes of obesity. A new research study, though, may have uncovered a remarkable mechanism–essentially a biological on/off switch for obesity. The work, which was published yesterday in the journal Cell, could help researchers develop better therapies to combat obesity.
Their idea is based on epigenetics–the concept that things like your height, weight, and other physical traits are based on not just what genes you inherit, but also the interaction of those genes with the environment you live in. Depending on that interaction, certain genes can turn on or off other genes–one of the main reasons why identical twins sometimes don’t look so identical.
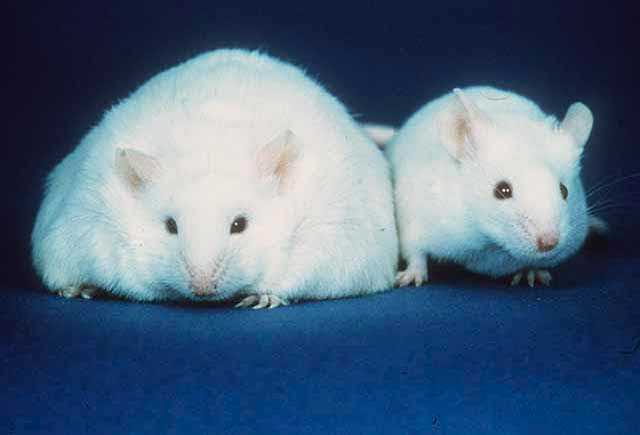
The researchers focused on a particular gene, named Trim28, which they found affected weight in mice–making them either lean or obese, but nothing in between. To understand Trim28 in humans, they studied 13 sets of identical twins in which one twin was obese and the other was lean. The researchers found less activity of Trim28 in the obese twins’ cells compared to their lean twin.
Scientists already knew that Trim28 can affect other genes that influence weight, so the researchers concluded that Trim28 may act as an epigenetic switch to either turn obesity on or off by suppressing or activating a set of genes that control weight.
This is a new way of thinking about how epigenetics influences obesity. Currently, many researchers think that epigenetics does influence weight but only in small amounts–nothing that would cause a person to become either lean or obese. This new idea would mean that obesity is either turned completely on or completely off–which gives reason to why one identical twin is obese while the other isn’t.
According to the CDC and National Institutes of Health, more than one in three adults in the United States are obese. By understanding the mechanisms through which obesity arises, researchers might be able to develop better treatments for the disease. (Back in 2013, the American Medical Association (AMA) officially recognized obesity as a disease, a classification that has likely given rise to increased research.)
While this switch seems promising, the researchers acknowledge that first they need to better understand how, when, and why the switch can be flipped on or off, which would direct what treatments for obesity could look like.
“Our next major goal is to see whether we can modify this process, whether we can turn the disease switch on or off by supplementing diet, minimizing stress, or giving epigenetically relevant pro-drugs,” says Andrew Pospisilik, one of the study’s authors, in a press release. “The hope is that we can permanently flip the system back to lean in one shot.”
