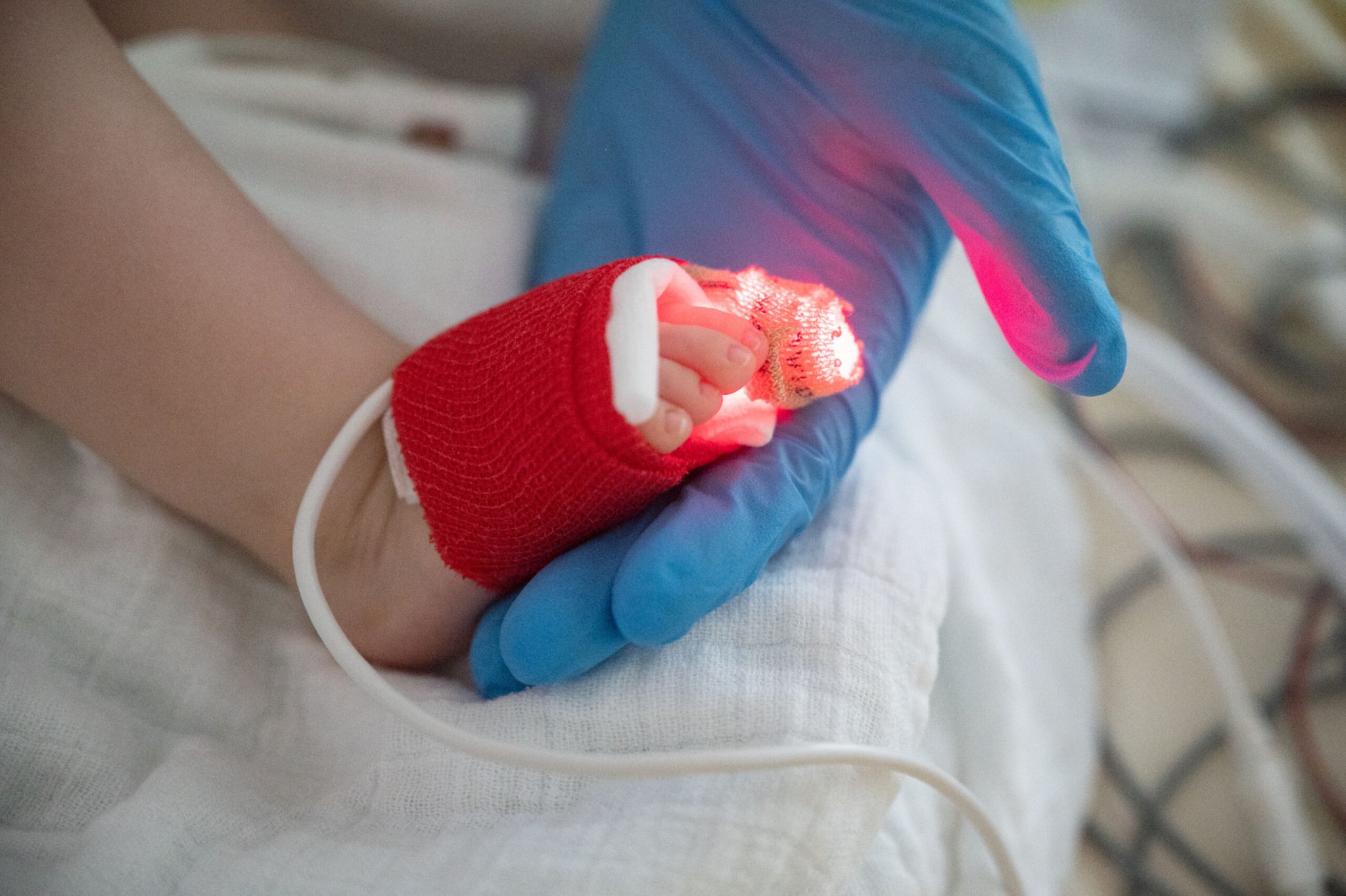

On Tuesday, Pfizer announced positive results from the trials for their respiratory syncytial virus (RSV) vaccine. Pregnant mothers early in their third trimester can receive the vaccine with the goal of protecting vulnerable infants from the virus in the first six months after birth. This is often when babies are most vulnerable to severe illness from RSV.
RSV is a common respiratory illness that is regularly seen during the fall and winter months. Most of those who contract it have similar symptoms to the common cold, but the virus can be life-threatening in young infants who have smaller airways. It is also a leading cause of hospitalization for babies. RSV is currently causing an unusually early spike in cases, overwhelming hospitals in many states. “It all has a very COVID-esque feel to it,” Meghan Bernier, the medical director of the pediatric intensive care unit at the Johns Hopkins Children’s Center in Baltimore, told The New York Times. “This is the pediatrician’s COVID. This is our March 2020.”
[Related: Is it flu or RSV? It can be tough to tell.]
According to the trial results, the vaccine appeared to be roughly 80 percent effective at preventing severe RSV disease infants in the first three months of life. It also cut a baby’s risk of needing to see a doctor due to infection in the first six months by half, and was 69 percent effective in preventing severe cases over six months.
The pharmaceutical company plans to apply for approval by the Food and Drug Administration (FDA) before the end of the year, with hopes that the vaccine could be available as early as next winter.
If approved, the vaccine will be the first RSV vaccine and the first new product related to the virus in more than 20 years. In March, the FDA designated Pfizer’s RSV vaccine a breakthrough therapy—a status that should speed up the review.
“We are thrilled by these data as this is the first-ever investigational vaccine shown to help protect newborns against severe RSV-related respiratory illness immediately at birth,” Annaliesa Anderson, senior vice president and chief scientific officer of vaccine research and development at Pfizer, said in a statement. “These data reinforce Pfizer’s resolve to bring our expertise in the research and development of innovative vaccines to address critical public health needs using new approaches and technologies.”
Pfizer said in the release that there were no major safety concerns for both vaccinated individuals and babies, and the data would continue to be closely scrutinized.
A total of 7,400 pregnant people participated in the trial, and the infants were followed for at least a year. Babies were considered to have severe RSV if they were breathing very rapidly (more than 70 breaths per minute in a 2-month-old), if their blood oxygen levels fell below 93 percent, if they required high-flow oxygen, if they were admitted to the intensive care unit (ICU), or if they lost consciousness.
[Related: Flu and RSV hybrid virus studied in a lab for the first time.]
The researchers in the trial also measured whether the shots prevented infant medical visits caused by RSV. It cut the need for infants to need to see a doctor by an average of more than 50 percent when compared with a placebo, which is not statistically significant. The company acknowledged in the release that the vaccine missed that particular goalpost.
However, in an interview with CNN, William Gruber, Pfizer’s senior vice president of vaccine clinical research and development, said that a 50 percent reduction in doctor visits due to RSV is still likely to be a noticeable and important benefit in the real world. “This is clearly sufficient and frankly, great news, for filing for our approval,” he said.
Maternal vaccines like this one provide an unborn baby with antibodies naturally passed down during pregnancy and provides a temporary, but immediate, bit of protection. Currently, vaccines for tetanus, pertussis, diphtheria, and the flu can be given to mothers during pregnancy.
Major pharmaceutical groups may make two additional tools to prevent RSV in infants available soon, as long as regulators agree they are are both effective and safe. In trials of a treatment from AstraZeneca and Sanofi called nirsevimab, a single dose of a monoclonal antibody could protect infants from RSV for five months. The drug was recently recommended for approval in Europe, according to a statement from AstraZeneca.
Additionally, two vaccines for older adults (from Pfizer and GSK) have also shown success against the virus.
