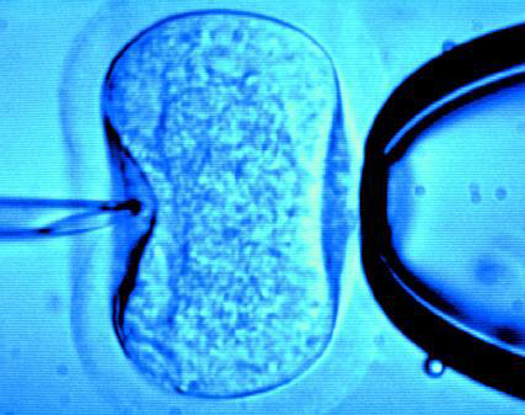

Five months ago, on April 6th of this year, a boy born to a Jordanian couple became the first baby born in the world using a new in-vitro fertilization technique that uses the DNA material from two women and one man, according to a report out today in New Scientist.
A U.S. team of doctors assisted with the birth, which took place in Mexico, according to New Scientist, as the technique has not been approved in the United States. However, its overwhelming success could help the approval process in the United States to be green-lit by the FDA soon.
The couple decided to go through with the technique after they found out that the baby boy’s mother is a carrier for Leigh syndrome, a fatal disease that afflicted her first two children; the first died at age six from the disease, and the second at just eight months. The disease-causing mutation is found in the mother’s mitochondria, and the three-parent technique avoided using her mitochondria all together.
The technique, which is called pronuclear transfer, typically involves fertilizing two eggs, one from the donor and one from the mother, with the same man’s sperm. Then, just before the eggs begin dividing, the nucleus (which contains all the genetic material except for the disease-carrying mitochondrial DNA) is removed from both eggs, and the nucleus from the mother’s egg is placed into the donor egg. But in this case, due to religious reasons, the couple opted for a different technique, called spindle nuclear transfer, in which the same nuclei swapping occurs, but only the donor’s egg is fertilized. The baby was born, healthy, with less than one percent of his mitochondria carrying the mutation, New Scientist reports.
Back in the 90s, scientists experimented with another technique that used three-parent babies where they injected donor mitochondrial DNA and sperm into a woman’s egg. However, the technique caused genetic diseases, likely from having a mix of two different mitochondrial donors, and was banned.
There are still obstacles before this new technique is approved. As we reported last year, many groups are concerned that this could lead the way for designer babies, where for example, parents could choose what color hair or eyes their child will certainly have. But researchers have strongly emphasized that, similar to gene-editing technologies like CRISPR-Cas9, the technique is for therapeutic use only, as it was in this case.
Safety of the procedure itself is another concern, but a review published in the journal Nature in June deemed the technique safe, and that it significantly reduces, though doesn’t guarantee 100 percent, the chances of passing fatal disease-causing mitochondrial mutations onto the carrier’s child.
Going forward, doctors and researchers will follow the baby to ensure that his levels of the mitochondrial mutation remain as low as they are now, and it’s likely the FDA could take his case into consideration in deciding whether or not to approve the technique’s use in the U.S.
