
This article was originally featured on High Country News.
Marin Hambley was working as a groundskeeper in Chico, California, when the first plumes of what would become the deadliest fire in the state’s history appeared on the horizon. It was Nov. 8, 2018.
Initially, all Hambley could see of the Camp Fire was a “little puff of cloud”—a sight not uncommon in the northeastern reaches of the Sacramento Valley, where summer temperatures routinely surpass 100 degrees Fahrenheit. But by midafternoon, “the sky was totally black and just dropping chunks of ash,” said Hambley.
Many residents evacuated; Hambley chose to stay. This area had been heavily impacted by the opioid crisis, and Hambley’s experience with harm reduction, a practice centered on minimizing the negative outcomes of drug use, made them acutely aware of the need to help people with substance abuse disorders. Additionally, their perspective as a queer and trans person led them to believe that they could be especially helpful to the marginalized populations that are often overlooked during disasters.
Since 2006, Butte County, where Paradise and Chico are located, has consistently been among the top three counties in the state for hospitalizations from opioid-related overdoses, with an annual rate between 2.75 and 5 times the state’s average.
In the hours after the plumes first appeared, Hambley heard about a pop-up encampment in an empty lot wedged between a busy throughway and the local Walmart. Hundreds of mostly low-income people had flocked there, fleeing the fire, and community organizers were distributing food, water and clothing. Meanwhile, those with means stayed in hotel rooms and Airbnbs or left the area entirely.
At the time, the county lacked official harm reduction infrastructure. Hambley and other organizers had to locate and distribute supplies on their own. Without the required certification, their activities weren’t technically legal, but Hambley said that was a risk they were willing to take. While the group had received a grant for purchasing Narcan—the overdose-preventing nasal spray approved for over-the-counter use last March—they had to obtain syringes, needles, cotton swabs and fentanyl test strips from groups elsewhere in the state. “We were all kind of underground,” Hambley said, noting that they smuggled backpacks stuffed with Narcan into Red Cross-operated shelters, where drug use was prohibited, though widely practiced.
At the Walmart encampment and other shelters, Hambley witnessed a disturbing rise in overdoses following the colossal Camp Fire, which ultimately killed at least 85 people and devoured nearly 240 square miles. A local paramedic noted that in the weeks following the fire, overdoses went from being a weekly occurrence to a daily one. And with a rate of 17 deaths per 100,000 residents, for the first time the Paradise area experienced a higher rate of opioid-related overdose deaths in 2018 than any other zip code in Butte County. Hambley said that’s because disasters cause both acute stress and chronic uncertainty, which can lead to more reactive and less managed drug use. “The chaos around you often precedes more chaotic (drug) use,” they said.
Across the Western U.S., climate disasters compound the devastation already caused by the deepening addiction crisis. Wildfires and floods breed anxiety, despair and isolation, all of which can exacerbate substance use. “Your house burns down, your community burns down, your school burns down—of course, you look for an escape,” said Sarah Windels, a co-founder of Bridge, a California-based program that promotes access to substance-use disorder treatment.
Beyond that, climate disasters halt addiction treatment programs and derail critical medication supply chains—all factors that heighten the risk of overdose, including for people who legally use opioids. This is especially true in rural areas, where fewer health-care providers are available, and patients often need to travel substantial distances to receive care. After a massive fire or flood, when local pharmacies and clinics may be closed, a person who is prescribed opioids for chronic pain or who is undergoing medication-assisted treatment (MAT) to curb their addiction may be forced to acquire a substitute illegally. If that supply has a higher potency than they are used to or, as is increasingly common, is laced with fentanyl, that individual is at a high risk of overdosing.
“Your house burns down, your community burns down, your school burns down — of course, you look for an escape.”
The data suggests that the connection between climate-induced disasters and overdoses is neither occasional nor individual, but seasonal and increasingly predictable. For instance, overdose rates are increasing every year across the nation, but in California, at least, they peak at the height of fire season. According to the California Overdose Surveillance Dashboard, emergency department visits for opioid-related overdoses have topped out during the third quarter of every year since 2018. And in 2020, the counties most affected by the vast August Complex Fire saw a surge in overdose deaths while the wildfire burned.
From the foothills of the California Sierras, to the floodplains of New Mexico, to the high Rockies in Colorado, these events are also forcing harm reduction workers to adapt their approaches to match their specific surroundings.
In Albuquerque, New Mexico, for example, extreme weather during the summer months accelerates overdose rates, said Ashley Charzuk, the executive director of the New Mexico Harm Reduction Collaborative, although the reasons differ from those in regions affected by wildfires. In Charzuk’s experience, people who use intravenous drugs can find veins more easily when it’s hot, owing to vasodilation, and this can lead to more frequent and potent use. What’s more, those who use stimulants are at greater risk of overamping, which is different from overdosing. “Your body temperature goes up when you’re using methamphetamine,” said Charzuk. When paired with high environmental temperatures, Charzuk said, overamping can lead to heart attack, stroke or other complications.
As heat waves get more extreme, Charzuk and her colleagues prioritize educating people about the risks of drug use when it’s hot out.
“We remind people … that heat plays into so many different metabolic factors,” said Charzuk. “If you’ve been out in the heat all day and you’ve been sweating, then you are going to be dehydrated, and anything that impacts your body like that is going to give you less of a defense.”
As someone who uses drugs and has experienced homelessness in the past, Charzuk has “met some of the same challenges that (program) participants meet on a daily basis,” she said.
Harm reduction workers are also at risk. In the summer of 2021, while handing out water in a local park, Charzuk was overcome by symptoms of heat stroke that kept her out of the field for days. “I feel like I learned a little bit more on how to take care of the people that are on my team as well as myself,” she said.
For Hambley, such incidents speak to how important it is for harm reduction workers to think about their own physical and mental health during crises, “or else everyone will burn out,” they said.
That tension came to a head for Arianna Campbell in the summer of 2021, when the Caldor Fire threatened to raze her community in Placerville, California, 90 miles southeast of Chico. As the flames approached, Campbell’s husband, a retired firefighter, suggested Campbell pack a go box. It was the first time he had ever done so.
“He had some indications that this was going to be a very big one,” said Campbell; in fact, the fire would go on to burn over 200,000 acres and more than 1,000 buildings.
But Campbell, a physician assistant, knew that she would be needed at the local hospital. Crises like wildfires strain emergency departments, Campbell explained, which are flooded by people with injuries, respiratory problems or other medical issues. This is especially likely for those who lack stable housing or have a substance use disorder. “If you’re someone who uses drugs, you may not necessarily have a lot of options,” Campbell said.
In Placerville, Campbell helped her hospital become one of the country’s first rural sites to offer buprenorphine, a medication that helps curb opioid addiction. “If someone is being treated on buprenorphine and there is a lapse in treatment, they are at close to three times the risk of dying,” she said, “because it puts them at such high risk of return to use and overdose.”
Maggie Seldeen, who describes herself as a practicing drug user, founded High Rockies Harm Reduction to address the dearth of safe injection supplies in the region surrounding Aspen, Colorado. Overdoses from opioids, most notably fentanyl, have skyrocketed in the state since the start of the pandemic. For Seldeen—who used cocaine and heroin intravenously for years, starting as a freshman in high school, and who has seen numerous friends contract hepatitis—practicing harm reduction through the use of clean needles and fresh syringes is critically important. But more frequent wildfires and landslides affected the area’s already strained supply chain.
“A lot of people of color, a lot of queer and trans folks, a lot of poor folks already understand the ways the system fails them.”
That puts the lives of people who use drugs at risk, she said. In 2020, for instance, the Grizzly Creek Fire meant that I-70 in Glenwood Canyon—45 miles north of Aspen, and a critical juncture on the route from Aspen to Denver, more than a three-hour drive away—was closed for two weeks.
“It gets really scary,” said Seldeen, who spoke about how the anxiety provoked by wildfires can push her and others to use substances as coping mechanisms.
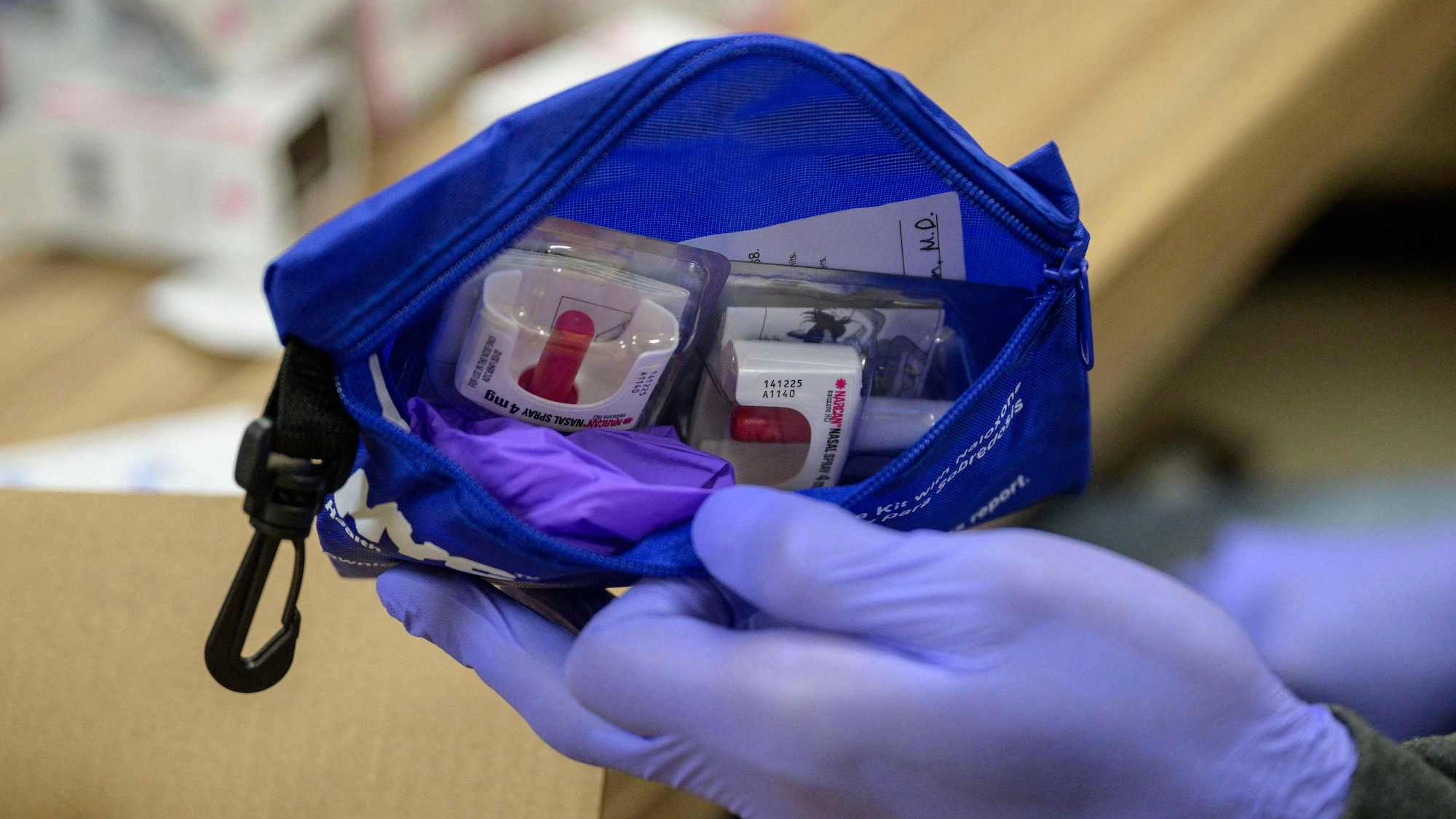
Now, Seldeen always has a go bag in her car when she is in the field in the summer months. It holds important personal documents, water, Narcan and first aid supplies, in case she encounters people who need help using drugs safely or reversing an overdose during an evacuation. Her hope is to create a network of people in the Rockies who are knowledgeable about—and prepared for—reducing the risks of drug use. Those connections, she says, will become increasingly important in a future that involves more climate events.
Seldeen isn’t alone in seeing the importance of community in facing the dueling crises of addiction and climate change. Back in Chico, Hambley now chairs the Northern Valley Harm Reduction Coalition, which Hambley helped grow in the wake of the Camp Fire, determined to continue the collective approach to harm reduction that came out of that disaster. “This is a community response,” they said. “The networks that we have are strong.”
The embers of the Camp Fire had barely cooled in March 2020, when the Chico network had to mobilize once again to prevent overdoses during the statewide COVID-19 lockdown.
“This is a marathon,” Hambley said, explaining how their queer identity and personal experience living on the margins have given them the tools to build a community that will rise to the challenge.
“A lot of people of color, a lot of queer and trans folks, a lot of poor folks already understand the ways the system fails them,” Hambley said. “As a queer trans person, I’ve already learned how to create family and community and networks outside of my home. Those are skills I live with every day, so in moments of crisis, our skill sets actually become incredibly valuable.”
Robin Buller is a freelance journalist based in Oakland, California. She writes about health, equity and climate. Email her at robinmbuller@gmail.com.
