ZMapp: The Experimental Ebola Treatment Explained
How tobacco may help defeat one of the world’s deadliest viruses.
Last Saturday in Monrovia, Liberia, neighbors stood in the street trying to block officials as the Liberian Ministry of Health brought 37 bodies of Ebola victims to a small plot of recently purchased land. In the midst of the burial, the excavator failed, leaving a few gaping holes in the ground and a pile of plastic covered shrouds. The bodies were left in open pits filled with water until Sunday, when a new delivery of cadavers was set to arrive. Plastic gloves and other equipment used during the burials were abandoned nearby, putting the town’s residents at risk of infection.
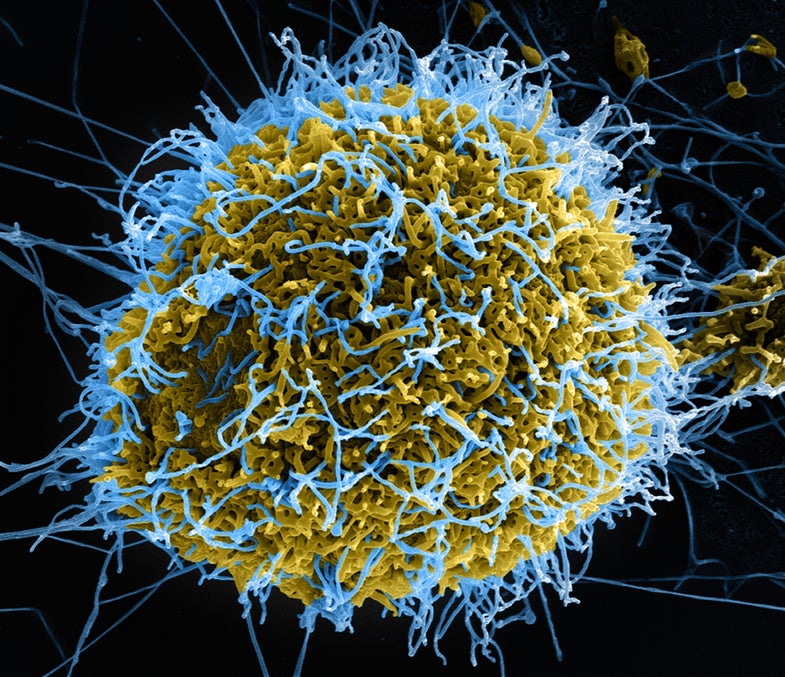
Ebola is one of the world’s most lethal diseases, causing vomiting, kidney and liver failure, and hemorrhagic bleeding. The fatality rate is up to 90 percent, and there’s currently no cure. Infection is spread by direct contact with animals or people who have the disease, which is why proper quarantine methods are so important. Unfortunately, as the burial scene in Monrovia last weekend demonstrates, health officials have struggled to contain the disease.
The virus is “moving faster than our efforts to control it.”
Over the last several weeks, an outbreak that started in Guinea in March has spread to Liberia, Nigeria, and Sierra Leone. More than 1,700 people have been infected, and the crisis ballooned last week, killing 170 people in just nine days. The virus is “moving faster than our efforts to control it,” said Dr. Margaret Chan, the director of the World Health Organization. If the situation continues to get worse, she said, the consequences could be “catastrophic.”
Deaths in the medical community have heightened the growing fear of the disease. Dr. Kent Brantly, an American physician who was working at Liberia’s Ebola Consolidated Case Management Center, is one of the most recent doctors to contract the disease. Heavily dressed in a gown, an apron, three pairs of gloves, a hood covering his strawberry-blonde hair, and green plastic protective eyewear, Brantly looked vaguely alien as he bent over patients’ beds. But all that gear didn’t keep him safe.
Shortly after Brantly tested positive, an American nurse, Nancy Writebol, was also diagnosed. Writebol was in charge of the wash-down station in the ELWA Hospital‘s 20-bed unit for Ebola patients. In the wash station, workers are sprayed with a chlorine solution, which is meant to decontaminate people entering and leaving the isolation ward. Neither Brently nor Writebol are sure just where they were exposed.
As news spread of the death of Samuel Brisbane, one of Liberia’s leading Ebola doctors, Brantly was evacuated in a special isolation plane back to the Dobbins Air Force Base in Georgia. Before leaving Liberia, in one of those strange twists of fate, he’d received a blood infusion from one of his 14-year-old patients who had survived the disease. The young boy, “wanted to be able to help the doctor that saved his life,” Brantly’s employer said. There are tentative findings to suggest blood transfusions from survivors may provide new patients helpful antibodies, but the strategy hasn’t been thoroughly tested.
Writebol was also given an experimental procedure, a dose of an untested serum. Initially there was only enough of the drug for one patient, and Brantly insisted it go to Writebol, who was in worse condition, but he’s since been treated with the drug also. Raising the question of who has access to top-quality care, the Americans are the only two patients who have been given the medicine, which had previously only been tested in lab animals.
The drug, ZMapp, is actually the collaboration between an American company, Mapp Biopharmaceutical, and a Canadian company funded by the Public Health Agency of Canada, who were working on similar projects when the outbreak hit. Mapp employs just nine people and has been financed only by the U.S. government, but they’re trying to figure out how to scale up quickly. Larry Zeitlin, Mapp’s president, told the New York Times, “We are discussing with the FDA the right path to make the drug available as quickly as possible.”
ZMapp itself is made up of proteins called monoclonal antibodies, which bind to the Ebola virus rendering it harmless. The drug is made by infecting mice with a protein from the Ebola virus, and then modifying the mice’s antibodies to more closely resemble human ones.
The results then need to be produced in large volumes, so scientists have turned to an interesting ally: plants. A gene from the modified antibodies is introduced to the leaves of tobacco plants, via a system developed by Icon Genetics. The leaves then produce the intended monoclonal “plantibody” proteins. It only takes about a week before the leaves can be harvested and the protein extracted and purified. Plus, it’s inexpensive compared to the traditional method of growing these genetically modified mouse cells in labs.
Currently, these modified antibodies are being grown in Kentucky tobacco plants by the tobacco company Reynold American. (Other industry giants, like Philip Morris, are also investing in medical plant-based technology.) “Pharming,” as the process is known, is particularly useful because it’s easier to produce proteins in higher volumes. “It is grown in a greenhouse, and you can manufacture kilograms of the materials,” Erica Ollmann Saphire, a professor at the Scripps Research Institute told Reuters.

But there are some challenges in scaling up the serum production, starting with the fact that clinical trials haven’t been run, and the Food and Drug Administration (FDA) still hasn’t approved the procedure. Plus, four out of seven monkeys treated with ZMapp in a trial last year still died of Ebola. How quickly the plantibodies can be produced also depends on Reynolds American, which may need several months to expand their facilities; the tobacco plants have to mature for about a month before they’re suitable for the procedure.
This frenzy highlights a significant problem with the way pharmaceutical research and development currently works: Because Ebola was so rare, there wasn’t a financial incentive for big companies to work on finding a cure before this outbreak occurred. Many more may perish before the serum comes online.
In the meantime at least, both Brantley and Writebol’s conditions are improving. Dr. Sanjay Gupta, CNN’s chief medical correspondent and an assistant professor of neurosurgery at Emory’s School of Medicine, said he thought the outbreak would continue to spread, adding, “We are going to see Ebola around the world.” But he thinks in the U.S. and other developed countries, it should be containable, an opinion the CDC echoes.
As Liberia totters toward renewed violence and Nigeria declares a state of emergency, the question is what will happen in the rest of the world—emphasizing how different access to medical care can be.